Anaphylaxis Alert: An affordable, wearable health monitoring device
ABSTRACT
The fear of anaphylaxis leads to stress and anxiety in individuals with severe allergies. An example of this is the fear of going into anaphylactic shock when around strangers who are unaware of how to treat the condition. The Anaphylaxis Alert was deigned to alleviate that fear. The device works by monitoring the saturated oxygen of the wearer. If the reading is too low (less than 94%), the Anaphylaxis Alert announces the situation verbally and begins to give commands to those around the victim. The pulse oximetry sensor, a MAX30102, was tested by the researcher running on a treadmill and then saturated oxygen was recorded using the design and a commercial pulseox for comparison. The data from the design and pulseox were significantly different (P<0.05). However, this difference can be accounted for in software. With more experimentation, the Anaphylaxis Alert could prove to be an inexpensive and effective health monitoring system.
INTRODUCTION.
Anaphylaxis is a life-threatening allergic reaction to antigens to which the body has developed a hypersensitivity. When this reaction occurs, the victim can have a variety of symptoms, including trouble breathing or swallowing, mental confusion, and abdominal pain (1). The rate of anaphylaxis in the United States is 49.8 cases per 100,000 person-years (2). Anaphylaxis requires immediate care and hospitalization (1).
A major concern for those with severe allergies is the possibility of going into anaphylactic shock without people who know about their condition being around them. The general public’s lack of knowledge of what an anaphylactic reaction looks like and how to treat it is one of the main causes of this fear. This problem is especially true with children. Children with allergies will tend not to have as much freedom as other children due to their condition. This problem is because of the uncertainty of the average person’s ability to treat anaphylaxis as well as a child’s inability to speak in situations like this. This fear is heightened when the child does not own any sort of communication device.
To address this fear, a device, named the Anaphylaxis Alert, was designed. When the wearer goes into anaphylaxis, the device will detect it and go through these steps: 1. It will announce, “Anaphylactic shock detected!” If the wearer does not press the button to confirm that they are going into anaphylaxis, or the button is not pressed after three minutes, the device will go to step two. 2. The device will begin to announce commands (e.g. “Check to see if the wearer has an epinephrine injector”) so people around can help. 3. Give directions on how to use the epinephrine injector and how to further assist. This device uses a pulse oximeter in order to know blood oxygen saturation (SpO2). This meter was chosen because in the event of an anaphylactic reaction, the wearer will have difficulty breathing, leading to a drop in saturated oxygen. This metric was chosen as it was deemed the most effective way to accurately detect an anaphylactic reaction with sensors on the outside of the body. Most other signs occur in the nervous system, such signs are difficult to evaluate with sensors.
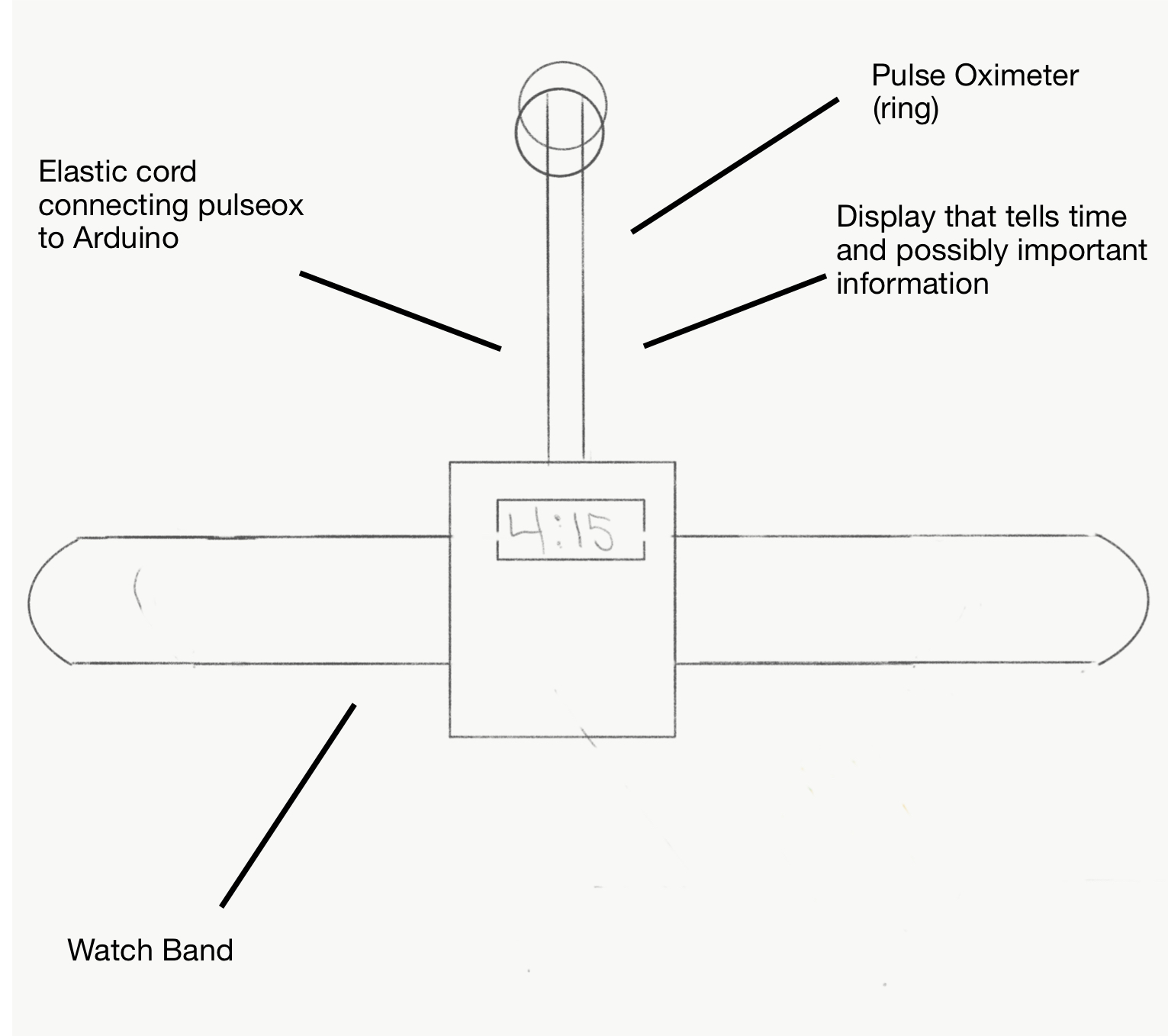
The device itself is a small unit similar to a watch (Fig 1). An elastic strap extends to the middle finger where the pulseox is placed for optimal readings. During design, portability and ergonomics were strongly considered in order to make the device as usable as possible on a regular basis. Another design consideration was expense. This novel device was created with the intention of having a low price in order to be accessible to all demographics. Additionally, the device sets itself apart from others through price and verbal warnings.
Figure 1. The original Anaphylaxis Alert schematic. Showing the basic qualities and dimensions.
MATERIALS AND METHODS.
Design components.
The four components of the design are: (1) an Elegoo Uno R3, (2) a Maxim Integrated MAXREFDES117#, (3 & 4) a speaker and an LED screen (neither of which have been finalized). The Elegoo Uno R3 is a microcontroller and a functional copy of the Arduino Uno. When the SpO2 value goes under the programmed threshold, the speaker begins to play commands. The display will also show the commands as well as the current SpO2 of the victim.
Data collection.
The pulseox sensor was compared to a SantaMedical SM-110 pulseox [Gurin Products, USA]. On the Arduino, the oximetry was measured multiple times per second. To compare it to the SM-110, the average reading of 20 data points was used. The pulseox sensor was tested by wearing the device on one hand and the SM-110 on the other after a strenuous run. Figure 2 shows the diagram of the arduino-sensor setup (Fig 2). This was the setup used when testing the pulseox sensor.
Figure 2. The pulseox to Uno connection used in initial oxygen saturation data collection.
Coding methods.
A large portion of the code used was modified example libraries (https://opensource.org/licenses/MIT). This code was comprised of the required pulseox library for identification and calibration as well as the code for the operation. The most significant modifications were the combination of example libraries to tell the device when to begin the process of announcing the anaphylactic shock. The purpose of the code was to turn the raw data from the sensor into SpO2 readings. For the SpO2 threshold, less than 94% was chosen because that is when most people start to experience problems due to lack of oxygen (3).
Data analysis.
Ten data points for the SM-110 and arduino were collected for a single test on an individual. The data was then added to a spreadsheet and an ANOVA was run on a TI-nspire CXS II [Texas Instruments, USA] to test variance.
RESULTS.
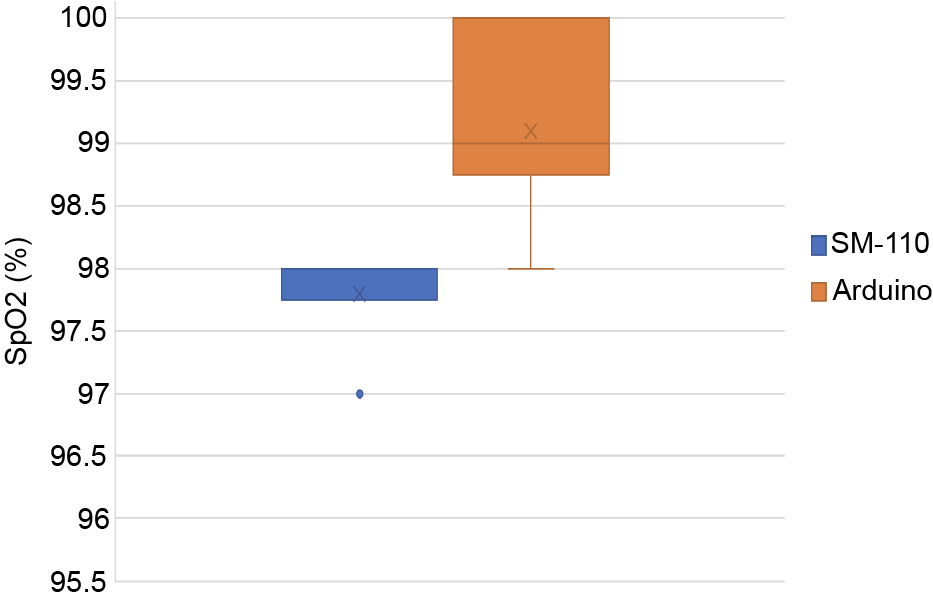
The SM-110 and Arduino SpO2 values were significantly different (P=0.00013). The Arduino was approximately 1% higher than the pulseox consistently. In real world applications, this small amount of difference is negligible. In the code, this can be fixed by simply adding a percent to the threshold (SpO2 <95%) as well as including a protocol where if it is lower than a certain amount for a time (e.g. lower than 96% for more than two minutes) the device will go into the alert mode.
The Arduino values varied more than the SM-110 (Arduino StDev: 0.0074, SM-110 StDev: 0.0042), which indicated that the SpO2 values were not as consistent (Fig 3).
Figure 3. Graph summarizing recorded SpO2 data. The data is represented by a box and whisker plot with the line/dot representing the minimum and x representing the median.
DISCUSSION.
With the appropriate technology, this design will be able to help people with severe allergies gain more freedom. Having the Anaphylaxis Alert will mean that in the event of anaphylactic shock, people in the area around will know what is occurring and how to assist. The Anaphylaxis Alert is not limited to those with allergies. The method of recognizing anaphylactic shock could be used in any medical emergency involving the respiratory system, such as COPD or severe asthma.
Limitations.
While the pulseox value was singular, the Arduino took multiple readings during the selected time, so an average was taken. This may have affected the Arduino’s readings as it is not known how frequently the SM-110 took readings. Additionally, the percent difference between the Arduino and SM-110 was most likely due to environmental factors in the Arduino sensor (such as external light, inconsistent pressure, etc.). This could be eliminated by covering the sensor in a glove finger to protect it from external stimuli. A glove finger would protect the sensor from variables as well as provide a constant pressure on the finger. More testing would need to be done in order to confirm that this would limit the number of variables.
Future design.
In order for the design to be optimized, a few changes will need to be made. To maintain the smaller watch shape, a Li-Ion battery would be used in conjunction with a flexible breadboard. The different battery will take up less room than the 9v as well as provide more power. The flexible breadboard will make the device more compact. Additionally, a different pulseox sensor with the ability to obtain readings from the wrist would eliminate the need for the ring around the middle finger. Another possibility for a better power system would be the integration of a supercapacitor instead of a battery. A supercapacitor would allow for additional streamlining due to its flexibility and versatility in shape. However, effective supercapacitors are currently still experimental and not yet readily available. Field testing with the device would need to be done in order to prove its abilities realistically.
CONCLUSION.
The Anaphylaxis Alert shows promise as an inexpensive and effective warning system for those with severe allergies or respiratory conditions. While other wearable warning devices on the market, such as the Apple Watch, start at more than $100, the Anaphylaxis Alert cost around $30-$40 to produce. The effectiveness and price of the Anaphylaxis Alert will allow a broad spectrum of demographics to have access to a potentially life-saving device.
ACKNOWLEDGMENTS.
I would like to thank Dr. Haag for his mentorship, Claire and Mia Elbon for their advice and support, and my parents, Mary and Andy for their constant devotion and unconditional support.
REFERENCES
- S. Shaker et al., Anaphylaxis-a 2020 practice parameter update, systematic review, and Grading of Recommendations, Assessment, Development and Evaluation (GRADE) analysis. J Allergy Clin Immunol 145, 1082-1123 (2020).
- J. Arnold, P. M. Williams, Anaphylaxis: Recognition and Management. Am. Fam. Physician 84, 1111-1118 (2011).
- W. H. Organization, Pulse Oximetry Training Manual (World Health Organization, 2011).
Posted by John Lee on Thursday, May 20, 2021 in May 2021.
Tags: Anaphylaxis, Medical Device, Wearable Technology